Macular Pucker & Macular Hole Treatment in Livingston and Morristown, NJ
What is A Macular Pucker?
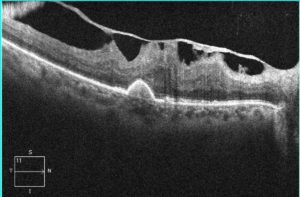
Pre-operative photograph of macular pucker with severe tractional pulling of the retina
A macular pucker, also known as an epiretinal membrane, premacular fibrosis, or cellophane maculopathy, is a thin layer of tissue membrane that forms over the macula, the central area of the retina that is responsible for our central and reading vision.
Macular puckers often develop on their own as part of the natural aging process. Small particles that have drifted into the vitreous (the gel that fills the eye) settle dependently on the surface of the macula and are slowly transformed into a scar tissue matrix. Membranes may also result from other eye conditions such as retinal tears and detachments, ocular inflammation, retinal vascular diseases, and trauma.
Many epiretinal membranes do not disrupt vision. Other membranes may mature and begin to contract on the surface of the macula causing wrinkles and folds. Distortion and loss of vision may result from the wrinkling and “puckering” of the macula. Symptoms may vary from mild blurry vision to severe central visual dysfunction.
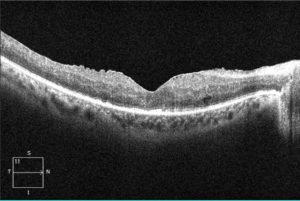
Post-operative photograph demonstrating the removal of scar tissue membrane and normalization of macular anatomy.
A patient who is sufficiently bothered by their distorted vision from macular pucker may benefit from surgical removal of their scar tissue membrane. A vitrectomy is performed in an outpatient surgery setting usually under a local anesthetic with mild sedation. Surgery is frequently extremely successful in helping patients to recover visual function previously impaired by macular pucker.
What is a Macular Hole?
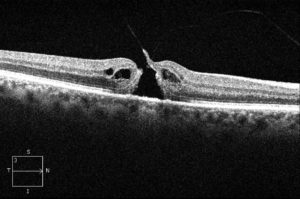
Full thickness macular hole.
A macular hole is a defect within the very center of the macula, the portion of the retina that is responsible for our fine detail oriented central vision. Reading and threading a needle are examples of “macular” vision. Macular holes almost always occur during the natural aging process. The vitreous gel within the eye undergoes changes that cause a tractional “pulling” around the center of the macula. The combination of these forces around the macula results in the formation of a hole. Other less common causes of macular holes may be related to trauma, a high degree of nearsightedness (myopia), and chronic swelling of the macula. Women are more likely to develop a macular hole.
At first, a macular hole may cause only a small blur or distorted area in the center of vision. As the hole grows and expands over several weeks to months, central vision progressively worsens. Peripheral vision is not affected and there is no risk of blindness. The duration and size of your macular hole will determine the level of visual recovery following repair. For this reason, prompt surgical intervention following diagnosis is recommended.
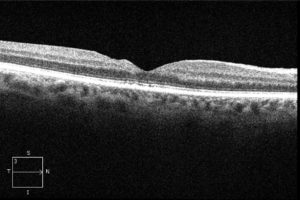
Resolution of macular hole following vitrectomy surgery.
Surgery is extremely effective in the treatment of macular holes. A vitrectomy is performed on an outpatient basis. Removal of the vitreous gel and dissection and peeling of the “tractional” macular membrane is completed under surgical microscopic control. A gas bubble is injected into the eye to help promote closure of the macular hole. Face down head positioning for several days following surgery will enable the bubble within the eye to remain in constant contact with the macula. The gas bubble acts as an internal bandage and is crucial to maximize the rate of surgical success. You may not fly in an airplane or travel to high altitudes with a gas bubble in your eye. The change in air pressure may result in a dangerous increase in the pressure within your eye. Our eye doctors will notify you when it is safe to travel following surgery.