Retinal Tears & Detachment Treatment in Livingston and Morristown, NJ
The vitreous gel fills the inner two-thirds of the eye. The vitreous is firmly attached to the retina, the inner lining of nerve tissue within the eye that is responsible for “transducing” light rays into nerve signals. As we get older, the vitreous gel begins to undergo age-related changes, and it may separate from the retina. Although this may result symptomatically in nothing more than a few floaters, sufficient pulling of the vitreous on the retina may occasionally result in a retinal tear.
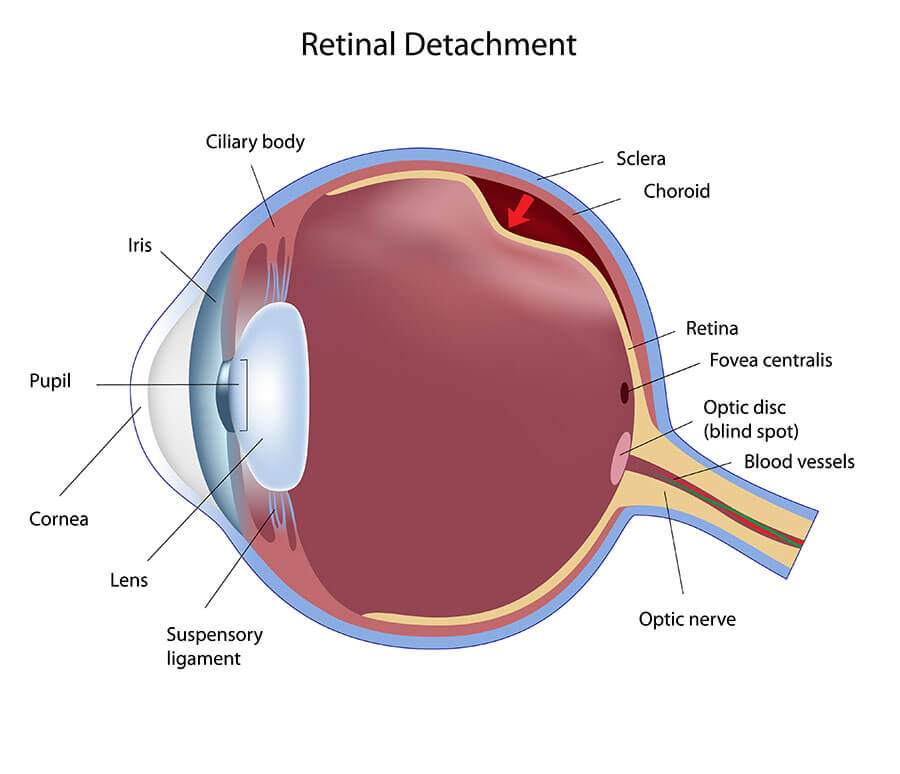
If vitreous fluid passes through the retinal tear and collects under the retina, causing a physical separation between the retina and its underlying supporting cellular layers, a retinal detachment will occur. Retinal detachments may cause significant and progressive vision loss and require surgical intervention for repair. Ideally, retinal tears can be identified and treated with either laser surgery or cryotherapy prior to the development of retinal detachment.
Conditions that may increase the risk for retinal tearing and detachment include, nearsightedness, congenital or acquired peripheral retinal thinning, family history of retinal tears and detachment, intraocular surgery such as cataract surgery, history of retinal tear or detachment in the fellow eye, and trauma.
A special type of retinal detachment may occur in diabetic patients and patients with chronic or recurrent retinal detachment. Scar tissue may cause tractional pulling on the retina, resulting in the loss of properly functioning retinal tissue. Vitrectomy in these patients will often result in stabilization of the disease as well as significant improvement in vision.
Signs and symptoms of retinal tears and detachment include flashing lights, floaters, a sense that a veil or curtain is obstructing your peripheral field or side vision, and a sudden drop in the quality of your central vision. If you experience any of these symptoms, please call our office immediately. Early intervention may help to preserve your vision.
What are the Treatment Options for Retina Surgery?
A retinal tear diagnosed by your physician may be treated in the office by laser surgery or cryosurgery to create a barrier to prevent further progression to a retinal detachment. These procedures are extremely well tolerated under mild local anesthesia. Patients will be asked to return to the office for a routine follow-up to determine if any additional retinal tears have developed.
There are several methods currently used to repair a retinal detachment. An in-office procedure known as pneumatic retinopexy may be performed if the configuration of the retinal detachment is suitable for this repair. A bubble of gas is injected into the eye. Appropriate head positioning is crucial to maximizing the rate of surgical success. Laser and/or cryosurgery are used to reduce further the risk of retinal re-detachment.
Scleral buckling surgery is performed in the operating room. A flexible band known as a scleral buckle is sutured to the back of the eye wall to counteract the intraocular forces that are acting to pull the retina from its normal position.
Vitrectomy for repair of a retinal detachment is similarly performed in the operating room setting, often in conjunction with a scleral buckle. Vitrectomy means “removal of vitreous,” the clear jelly-like substance that fills the inner portion of the eye. Using an operating microscope, your surgeon will enter through small ports on the surface of your eye and remove the vitreous and any accumulated blood, scar tissue, inflammatory debris or foreign bodies that may have developed secondary to a variety of clinical conditions. Very fine instruments such as picks, micro-forceps, scissors, and knives are used to complete the vitrectomy surgical procedures. Replacement of the vitreous gel with a physiologic salt solution, intraocular gas, or a long-term tamponade agent such as silicone oil may be performed depending on the severity of your detachment. Laser surgery is commonly used as an adjunctive procedure during vitrectomy surgery to help “seal” the retina in place. Appropriate head positioning is crucial if an intraocular gas is used. You may not fly in an airplane or travel to high altitudes with a gas bubble in your eye. The change in air pressure may result in a dangerous increase in the pressure within your eye. Our eye doctors will notify you when it is safe to fly or to travel to higher altitudes.
Visit our contact us page and schedule an appointment at one of our two locations in Morristown and Livingston, NJ.